What We're Covering
Negotiated Rates data includes multiple dollar amounts for the exact same procedure—charges, allowed amounts, paid amounts, and patient responsibility. This guide breaks down what each term means and reveals exactly which ones should drive your revenue and contracting decisions.
Why This Matters
When you are analyzing healthcare price transparency data or preparing for contract negotiations, you need to know which numbers to focus on. Focusing on the wrong metric wastes your time and skews your financial reality. Tracking the right metric tells you whether you are truly competitive in your market.
The Four Numbers You Will See
To understand your revenue cycle, you need to differentiate between these four core pricing metrics:
1. What is a charge?
The charge is the list price found in your hospital's chargemaster. For example, a facility might charge $10,000 for a knee MRI. Almost nobody pays this amount. It is an accounting artifact leftover from old negotiation tactics. It tells you absolutely nothing about your actual revenue or market competitiveness.
2. What is a Negotiated Rate, or Allowed Amount?
The allowed amount is the actual negotiated rate between your facility and the insurance payer. If Blue Cross agrees to pay $1,200 for that knee MRI, that $1,200 is your total recognized revenue for the case.
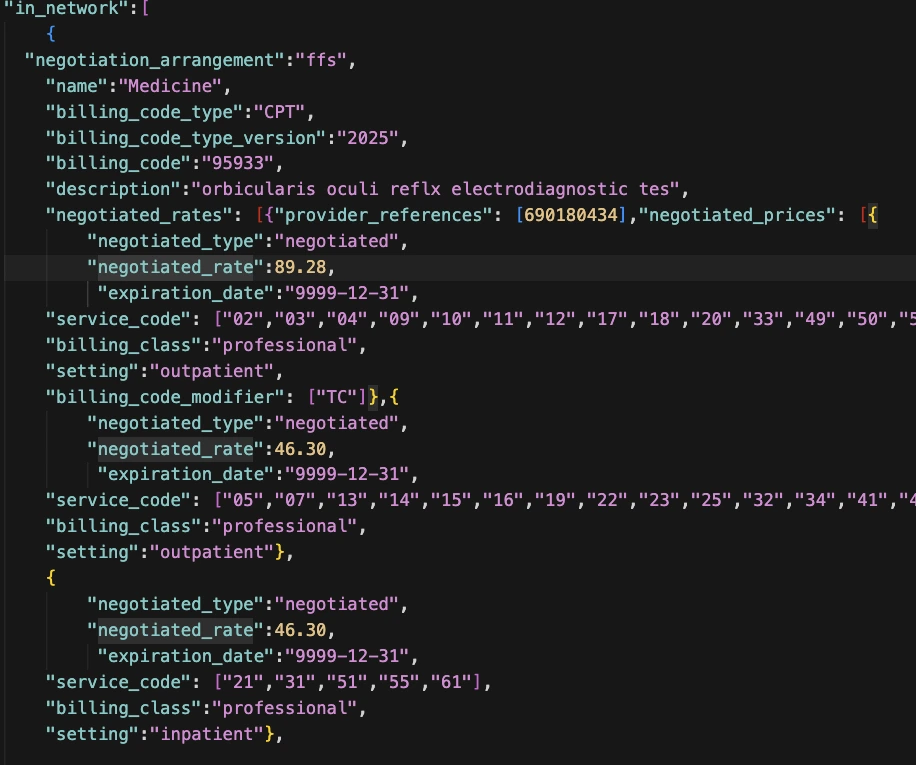
This is the most important number in price transparency files. When benchmarking against competitors or negotiating contracts, this is your baseline. If your facility's allowed amount is $1,200 and the competitor across town is getting $2,400 from the same payer, they are receiving double your revenue for the exact same work.
3. What is the Paid Amount?
The paid amount is what the insurance payer actually sends you after applying the patient's specific deductible, copay, and coinsurance. The paid amount fluctuates constantly based on each patient's benefit plan and where they are in their benefit year.
- If the allowed amount is $1,200 but the patient hasn't met their deductible, the payer sends $0.
- If the patient has a 20% coinsurance, the payer sends $960.
Because it varies case-by-case, the paid amount is not useful for understanding market rates or benchmarking. It merely dictates the payer's portion of the bill in one specific scenario.
4. What is the Patient Responsibility?
What the patient owes depends entirely on their specific plan design—their deductible, coinsurance percentage, out-of-pocket maximum, and timing within their benefit year. Two patients can get the same MRI at your facility under the same $1,200 allowed amount, yielding entirely different billing workflows. One patient may have hit their deductible (you collect $0 from them), while the other hasn't (you must collect the full $1,200 from them). Your total revenue remains the same, but your collection complexity changes.
How to Use This Data
The allowed amount or negotiated rate is your contracted revenue. It is comparable across facilities, consistent until your contract renews, and serves as the foundation for your financial planning. Everything else is simply downstream from that negotiated rate.
When you are analyzing pricing data, keep your focus on the allowed amount to drive these four key strategies:
- Benchmarking: Compare your allowed amounts against competing facilities for the same payer and service to understand your exact competitive position.
- Contract Negotiations: Use competitor allowed amounts to justify your rate increases. If you are contracted at $1,200 and a competitor is at $2,400 for the same payer, you have data-backed leverage.
- Revenue Forecasting: Base your financial projections strictly on allowed amounts, not chargemaster rates. You can then adjust for expected patient responsibility based on your facility's historical payer mix and collection rates.
- Payer Mix Strategy: Identify which insurance payers offer competitive allowed amounts and which fall short, allowing you to prioritize relationships with those paying more favorable rates.
